Key aspects
Research
NCD Research
Our community-based intervention aims at improving NCD care and expanding access to treatment.
Primary research is the starting point for any efficient and locally adapted health intervention. Balamu thereby follows the long-term goal of strengthening diagnosis and treatment in rural Uganda. We identify prevalence and risk factors, while evaluating models of health education. The team focuses on hypertension, diabetes, chronic kidney disease and COPD. These are the NCDs accounting for the majority of global deaths.
While our previous efforts relied on collecting self-reported data, in the coming years we will set up a longitudinal cohort. We will formally diagnose NCDs in the field and create a community-based referral system.
Education
Health education

We build on partnerships between health care providers, patients and families to provide patient-centered education as an essential component in NCD management.
Medical care that is sensitive to patients and administered in a respectful fashion leads to enhanced information sharing between all members of a treatment team. Patient-centered education has been shown to improve health outcomes and quality of life for patients with chronic diseases.
We ensure that patients receive comprehensive health education to participate in medical decision-making. This education encourages the population to adopt healthy behaviors. We make complex medical conditions easily understandable.
Our bilateral exchange provides medical professionals from Uganda, Germany and the US with a broader knowledge of global health issues and the discrepancies between countries.
We coordinate an annual bilateral exchange between Makerere University, Yale University and Charité Universitaetsmedizin Berlin. During this exchange medical students from Uganda get a chance to learn new skills, insights and methods. German and US students have the opportunity to learn about current global health issues and inequalities from a lower resource perspective.
Care
Community Health Workers

Sustainable models of care are crucial for creating long-term, positive health outcomes. Community-based interventions have proven to be successful at informing patients and ensuring access to remote areas.
We work with community health workers (CHWs) who sensitize the local population. CHWs test patients, refer them to the participating health centers and provide long-term care. CHWs can carry out a large part of the medically necessary examinations and thus relieve doctors.
CHWs have greatly contributed to the success of Balamu as the pillars of our community-based intervention. The training and further education of CHWs is a main target. We will leverage the successful CHW-delivered education we developed and add comprehensive testing, referral and follow-up in the community.
Objectives
We aim to consolidate, improve and expand the care for patients with NCDs. Our aim is to develop a model of care that can be adopted to different regions in Uganda and other low-middle-income countries.
Improving and expanding NCD care in rural Uganda
Development of NCD care through the integration and evaluation of a CHW-delivered treatment system. Evaluation of the quality of NCD care in rural Uganda.
Strengthening NCD training in Nakaseke, rural Uganda
Continuation of the education of health professionals by incorporating formal NCD training and expanding the joint exchange between Charité , Yale and Makerere University.
Developing infrastructure and sustainability
Development of infrastructure and sustainability by designing a digital system to improve quality of care and capacity. We will strengthen the visibility and support of our NCD program.
Accomplishments
Since 2016 we built a Center for NCD Research, Education and Care in Nakaseke district. We have successfully established a CHW-based NCD primary care system along a set of milestones:
Publications
CHW Effectiveness

Effectiveness of a community health worker-delivered care intervention for hypertension control in Uganda: study protocol for a stepped wedge, cluster randomized control trial
Ingenhoff, R., Nandawula, J., Siddharthan, T., Ssekitoleko, I., Munana, R., Bodnar, B. E., Weswa, I., Kirenga, B. J., Mutungi, G., van der Giet, M., Kalyesubula, R., & Knauf, F. (2022). Trials, 23(1), 440. https://doi.org/10.1186/s13063-022-06403-9
Cohort Study

The rural Uganda non-communicable disease (RUNCD) study: prevalence and risk factors of self-reported NCDs from a cross sectional survey
Siddharthan T, Kalyesubula R, Morgan B, Ermer T, Rabin TL, Kayongo A, Munana R, Anton N, Kast K, Schaeffner E, Kirenga B, Knauf F (2021). BMC Public Health21(1) :2036. doi: 10.1186/s12889-021-12123-7
Qualitative Research

Challenges to hypertension and diabetes management in rural Uganda: a qualitative study with patients, village health team members, and health care professionals
Chang, H., Hawley, N. L., Kalyesubula, R., Siddharthan, T., Checkley, W., Knauf, F., & Rabin, T. L. (2019). International journal for equity in health, 18(1), 38. https://doi.org/10.1186/s12939-019-0934-1
Patient-Centered Education

Implementation of Patient-Centered Education for Chronic-Disease Management in Uganda: An Effectiveness Study
Siddharthan, T., Rabin, T., Canavan, M. E., Nassali, F., Kirchhoff, P., Kalyesubula, R., Coca, S., Rastegar, A., & Knauf, F. (2016). PloS one, 11(11), e0166411. https://doi.org/10.1371/journal.pone.0166411
Nephrology and Global Health
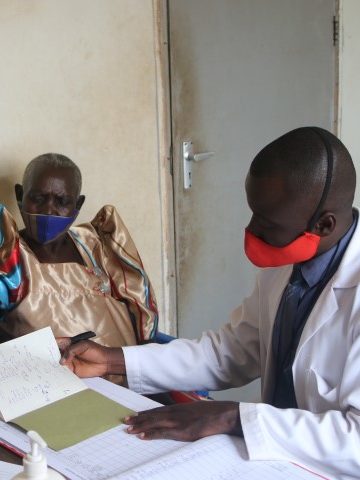
An interim report on the development of patient care in rural Uganda.
R. Ingenhoff, D. Ganten und F. Knauf.Nephrologie und Global Health? Ein Zwischenbericht über den Aufbau von Patientenversorgung im ländlichen Uganda. 2021; 50: 194-199. doi: 10.5414/NHX02177.

Acceptability of implementing hypertension specific health education by CHWs among people living with HIV/AIDS (PLWHA) in rural Uganda.
Batte, C., Mukisa, J., Rykiel, N., Mukunya, D., Checkley, W., Knauf, F., Kalyesubula, R. & Siddharthan, T. (2021). BMC Public Health 21, 1343. https://doi.org/10.1186/s12889-021-11411-6
Balamu Annual Report 2022

Summarising our results from the second year of this funding period by presenting our achievements.
Balamu Annual Report 2021

Summarising our results from the first year of this funding period, reflecting on NCD Resarch, Education and Care.
ACCESS Annual Report 2020

Reflecting on the activities of ACCESS in 2020, focusing on strengthening primary care and NCD screening in Nakaseke district.
